Substance use
Substance use
Substance use among children and youth can harm their physical and mental development. Early initiation of substance use (especially before the age of 14) is associated with a higher risk of developing problematic substance use or dependence later in life.1 For substances such as tobacco, e-cigarettes, alcohol, cannabis, opioids, and other products, Ontario public health units strive to prevent or delay substance use, reduce harms associated with substance use, and prevent problematic substance use.2 Specific to children and youth, health units have a mandate to ensure that youth have reduced access to tobacco products and e-cigarettes3, and to work with schools related to substance use prevention and harm reduction2. In Middlesex-London, over 98% of youth reported abstaining from cigarettes, while almost a third reported having used cannabis at least once.
The Substance Use topic contains data for the overall Middlesex-London population on tobacco, alcohol use, cannabis, and opioids and other substances.
| Tobacco | Drugs |
Tobacco
The Tobacco section contains data for the overall Middlesex-London population on smoking status, intentions to quit smoking, smoking abstinence, and exposure to second-hand smoke.
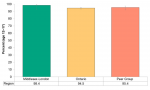
Over 98% of the youth population age 12–17 in Middlesex-London reported completely abstaining from cigarettes in their lifetime (Figure 13.5.1). The percentage in Middlesex-London was higher compared to Ontario (94.5%), but the difference was not statistically significant. Due to small sample sizes, socioeconomic factors such as income and education could not be examined for youth abstinence.
The Exposure to second-hand smoke section includes data on the percent of population (age 12+) exposed to second-hand smoke at home (Figure 5.1.9), or in a vehicle or outdoor space (Figure 5.1.10).
Interpretation
According to the 2017 Canadian Tobacco, Alcohol and Drugs Survey, the average age for which Canadians first smoked a cigarette was 16.4 years.4
Since 1977, the Centre for Addiction and Mental Health (CAMH) has conducted a survey of students in Ontario in grades 7 through 12 called the Ontario Student Drug Use and Health Survey (OSDUHS).5 The survey collects self-reported information from students about home and school life, physical health, mental health, antisocial behaviour and bullying, substance use and other risk behaviours. In the 2017 cycle of the survey, 7.0% of students reported using cigarettes, 5.4% smokeless (chewing tobacco), and 10.7% electronic cigarettes (vapour products) in the past year.6
Drugs
The Opioids and Other Substances section contains data for the overall Middlesex-London population on opioid-related deaths, opioid-related emergency department visits, and use of other substances.
Almost a third (31.9%) of youth (age 12–17) in Middlesex-London reported using cannabis in their lifetime in 2015/16, and 27.4% in the past 12 months (Figure 13.5.2).
Among the 10–14 age group in Middlesex-London, the rate of cannabis-related emergency department visits was 45.0 per 100,000 in 2017 (Figure 5.3.5). This rate was significantly lower compared to youth and young adults age 15–24 (269.9 per 100,000).
Among youth and young adults age 15–24, the rate of opioid-related emergency department visits was 152.9 per 100,000 in 2017; this rate was significantly lower compared to those age 25–44 (Figure 5.4.7).
Interpretation
The average age at which Canadians first experiment with substance use varies by substance. The Canadian Tobacco, Alcohol and Drugs Survey (CTADS) is a survey conducted every two years by Statistics Canada on behalf of Health Canada on tobacco, alcohol and drug use among Canadians age 15 years and older.7 According to the 2017 CTADS, the average age for which Canadians first: drank alcohol was 18.3 years, used cannabis was 18.6 years, and used other illegal drugs was 19.2 years. For youth age 15–19, alcohol is by far the most common substance used, followed by cannabis.4
In the 2017 cycle of the Ontario Student Drug Use and Health Survey (OSDUHS), 42.5% of Ontario students reported using alcohol and 19.0% reported using cannabis in the past year; for both substances, percentages were similar between males and females, and were higher for older grades (i.e., lowest among students in grade 7 and highest among students in grade 12).
Ontario Public Health Standards: Requirements for Programs, Services, and Accountability
Population Health Assessment and Surveillance Protocol, 2018
Substance Use Prevention and Harm Reduction Guideline, 2018
References:
1. Jordan CJ, Andersen SL. Sensitive Periods of Substance Abuse: Early Risk for the Transition to Dependence. Dev Cogn Neurosci [Internet]. 2017 [cited 2019 Jul 25];25:29–44. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5410194/ DOI: https://doi.org/10.1016/j.dcn.2016.10.004
2. Ministry of Health and Long-Term Care. Substance Use Prevention and Harm Reduction Guideline, 2018 [Internet]. Toronto, ON: Queen's Printer for Ontario, 2018 [cited 2019 Aug 12]. Available from: http://www.health.gov.on.ca/en/pro/programs/publichealth/oph_standards/d...
3. Ministry of Health and Long-Term Care. Ontario Public Health Standards: Requirements for Programs, Services, and Accountability [Internet]. Toronto, ON: Queen's Printer for Ontario, 2018 [cited 2019 Jul 30]. Available from: http://www.health.gov.on.ca/en/pro/programs/publichealth/oph_standards/d...
4. Statistics Canada. Canadian Tobacco, Alcohol and Drugs Survey, 2017 [Internet]. Ottawa, ON: Government of Canada; 2018 [cited 2019 Jul 25]. Available from: https://www150.statcan.gc.ca/n1/daily-quotidien/181030/dq181030b-eng.htm
5. Boak A, Hamilton HA, Adlaf EM, Henderson JL, Mann RE. The Mental Health and Well-Being of Ontario Students, 1991–2017: Detailed Findings from the Ontario Student Drug Use and Health Survey (OSDUHS) (CAMH Research Document Series No. 47) [Internet]. Toronto, ON: Centre for Addiction and Mental Health, 2018 [cited 2019 Jul 18]. Available from: https://www.camh.ca/-/media/files/pdf---osduhs/mental-health-and-well-be...
6. Boak A, Hamilton HA, Adlaf EM, Mann RE. Drug Use among Ontario Students, 1977–2017: Detailed Findings from the Ontario Student Drug Use and Health Survey (OSDUHS) (CAMH Research Document Series No. 46) [Internet]. Toronto, ON: Centre for Addiction and Mental Health, 2017 [cited 2019 Jul 18]. Available from: https://www.camh.ca/-/media/files/pdf---osduhs/drug-use-among-ontario-st...
7. Statistics Canada. Canadian Tobacco, Alcohol and Drugs Survey (CTADS): Summary of Results for 2017 [Internet]. Ottawa, ON: Government of Canada; 2019 [cited 2019 Oct 18]. Available from: https://www.canada.ca/en/health-canada/services/canadian-tobacco-alcohol...
Last modified on: November 7, 2019
Jargon Explained
Lifetime abstainer
Has never smoked a whole cigarette in lifetime.
Cannabis-related emergency department visit
These include visits for poisonings as well as cannabis-related mental health and behavioural reasons: acute intoxication; dependence; withdrawal; and, cannabis-related psychotic disorder.