Violence
Violence
Assault-related injury visits to the emergency department appear to be on the rise with increasing rates between 2015 and 2017 after showing a decline between 2009 and 2014. Males, younger populations and those in urban areas were more likely to have experienced an ED visit for injury.
Deaths rates due to assault were generally low in Middlesex-London in 2012 (1.6 per 100,000) and did not differ significantly from Ontario as a whole and the Peer Group. There was no significant difference over time. (Figure 4.7.1).
From 2009 to 2014 the rate of emergency department visits for assault (255.7 per 100,000) in Middlesex-London declined, but began to increase again to 2017 (325.6). The 2017 rate is similar to that seen in 2011. Rates of emergency department visits due to assault in Middlesex-London were similar to rates in the Peer Group, but higher than Ontario rates (Figure 4.7.2).
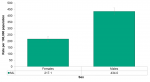
Males (434.0 per 100,000) had the highest ED visit rate for assault, nearly double and significantly higher than females (217.1) (Figure 4.7.3).
20-44 year olds had the highest rate of emergency department visits due to assault injury among all age groups followed by the 0-19 year old age group (not shown).
The rates of assault were significantly higher in urban (331.4 per 100,000) populations compared to rural (234.7) (Figure 4.7.4).
Interpretation:
Intentional injuries that are described here are those injuries that occur when someone brings harm to others. Examples include intimate partner and domestic violence, sexual assault, youth violence and child maltreatment. However, family and intimate partner violence is known to be chronically under estimated.1 There are many different factors that put individuals at risk for perpetration of violence. They can be societal or individual factors. Exposure to violence, drug and alcohol use in home, low parental involvement, lack of social involvement or commitment to school and diminished economic opportunities in the community are just some of the risk factors that have been identified for youth violence.2 Risk factors such as history of violent victimization and exposure to family violence reinforces the idea those who have been victimized are at risk to harm others. Similar to what was seen in Middlesex-London, data from a large nationwide US sample showed hospitalizations related to assault were higher in urban areas compared to rural areas.3
Population Health Assessment and Surveillance Protocol, 2018
References:
1.Public Health Agency of Canada [Internet]. Ottawa (ON): Government of Canada. Family Violence: How big is the problem in Canada? [modified 2018 May 31; cited 2019 Mar 12]; [about 4 screens]. Available from: https://www.canada.ca/en/public-health/services/health-promotion/stop-family-violence/problem-canada.html
2. David-Ferdon C, Vivolo-Kantor AM, Dahlberg LL, Marshall KJ, Rainford N, Hall JE. A comprehensive technical package for the prevention of youth violence and associated risk behaviors [Internet]. Atlanta (GA): National Centers for Disease Control and Prevention, National Center for Injury Prevention and Control; 2016 [cited 2019 Feb 14]. 64 p. Available from: https://www.cdc.gov/violenceprevention/pdf/yv-technicalpackage.pdf
3. Coben JH, Tiesman HM, Bossarte RM, Furbee PM. Rural-urban differences in injury hospitalizations in the U.S., 2004. Am J Prev Med [Internet]. 2009 Jan [cited 2019 Feb 13];36(1):49–55. Available from: https://www.ajpmonline.org/article/S0749-3797(08)00836-2/fulltext
Last modified on: March 15, 2019
Jargon Explained
Small counts:
The stability of a rate is dependent on the number of events that contribute to that rate. Therefore, rates in small populations are often unstable due to the relatively small number of events that occur each year. When comparing trends over time between Middlesex-London, the province and the Peer Group, we often see a larger fluctuation in rates locally than for Ontario, in which the trends are fairly smooth from year to year – this concept needs to be considered when interpreting the time trends and the confidence intervals in this resource.